India has been polio free since January 2011. Before the launch of polio immunisation campaigns in 1995, an estimated 50,000 to 100,000 polio cases were being reported annually, so that's quite an achievement. The near-eradication of polio in India was made possible by the strong ownership of the Government of India, and by the efforts of a number of actors in the health sector, including World Health Organisation (WHO), The United Nations Children's Fund (UNICEF) and Rotary International.

What I was in Delhi to ask about was how important was the contribution of the World Health Organisation in particular?
The answer is, pretty crucial. We were told so not just by the WHO country team, but also by national and state government partners, medical officers and the mothers of children benefitting from the immunisation programme...
... including Dr Pooja Sarin who proudly presented to us the clinic she runs in Mehrauli, Delhi. As she spoke she referred to a well-thumbed copy of the WHO Immunisation Handbook for Medical Officers. She also ended with a ringing endorsement of India's state-run facilities, which should all be compliant with WHO guidelines and global best practice; "My children were vaccinated in this clinic. I would always bring them to state-run clinics over private ones because I know that they follow WHO guidelines."
What WHO had produced on polio eradication was a set of practical guidance and training, specific to the Indian national context, for immunising all children against polio. WHO delivered the technical advice and expertise to help make the Government's target of attaining polio free status a reality. Importantly, what WHO and Indian medical staff learned along the way is also now being shared with other countries battling the same foe, for example during a recent WHO delegation to Nigeria.
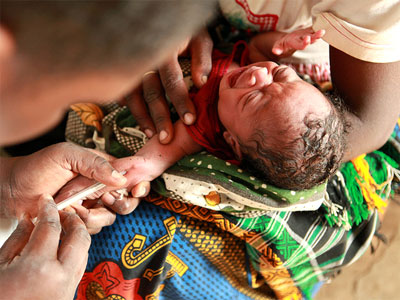
Immunisation programmes, including against polio, are of course just one aspect of the organisation's work in India.
The recently agreed WHO Country Cooperation Strategy has improved health and equity in India at its heart with three key objectives - i) supporting an improved Government of India role in global health; ii) promoting access to and utilisation of affordable, efficiently networked and sustainable services for the whole population; and iii) helping to confront the new epidemiological reality of India. WHO, along with agency partners in the UN Country Team, prioritises its delivery in the nine states in India with the highest proportion of people living in poverty – Odisha, Bihar, Chattisgarh, Madhya Pradesh, Jharkhand, Uttar Pradesh, Maharashtra, Assam and Rajasthan.
How WHO delivers on such an important set of objectives goes to the heart of what the UK and DFID expects from our development funding to the agency. India was an incredibly valuable context in which to consider the impact that a normative and standard setting agency like WHO can and should be having. These agencies play a vital role providing technical expertise, neutral advice and convening power, data and analysis, to help governments to meet international standards, and to deliver progress against MDG targets and on government poverty reduction and development plans. In India, WHO provides something that only agencies like this can - considerable support over a long time period to achieve significant outcomes that have wide a ranging impact. It took 15 years to near-eradicate polio in India following the initial adoption of WHO guidelines in 1995. The process was non-linear, with successes and setbacks, where anything less than full, robust support would have been insufficient.
To continue to succeed in this role, WHO needs to ensure that it is focusing on its proven comparative advantage, and monitoring its organisational effectiveness and delivery of results to demonstrate value for money from the funding it receives. DFID will be looking closely at these things when refreshing the Multilateral Aid Review (MAR) assessment of WHO next year.
So are the global standards and guidelines, researched and drafted in Geneva and across the world, important for achieving great things in world health? This was one tick in the credit column.

4 comments
Comment by Harsh Sahay posted on
Good Job 🙂
Comment by Anup Daniel.K posted on
who put up great show in india.thanks who
Comment by Shyla posted on
AWESOME!!!
Comment by penpa posted on
a good job done, which will change many peoples life....:-):-):-):-);-);-);-)